PROTECT Publication Analyzes the Impacts of Hurricanes Irma and Maria on Maternal Health
A new paper published in the Children journal of pediatrics and led by PROTECT trainee Irene Lafarga Previdi looks at the experiences of pregnant and post-partum women during and after hurricanes Irma and Maria. Irene, who is also the RCMI Center for Collaborative Research in Health Disparities Community Engagement Coordinator, led the publication with collaboration from researchers across different PROTECT projects and institutions. The paper’s analysis finds common themes among the women as related to pregnancy and birth challenges, access to basic services, and more.
After hurricanes Irma and Maria devastated Puerto Rico in 2017, PROTECT released a questionnaire to women who were pregnant during the hurricanes or became pregnant shortly after. The final open-ended question on the survey asked participants, “Is there anything else that you would like to share with us about your experience during or following Hurricanes Maria or Irma?” The analysis in this paper put 76 answers to this question through a coding process and identified common experiences related to the hurricanes.
Participants faced a variety of challenges. Several women had unplanned cesareans. One woman had increased blood pressure during her procedure due to stress that the hospital’s generator could stop working. Some participants gave birth at least two weeks before their due date. Others had trouble getting prenatal vitamins and important baby supplies in the leadup to giving birth. Like many on the island, some participants lost their homes and belongings, and the emotional impact of this was amplified by the stress of being unable to welcome their babies to a safe home.
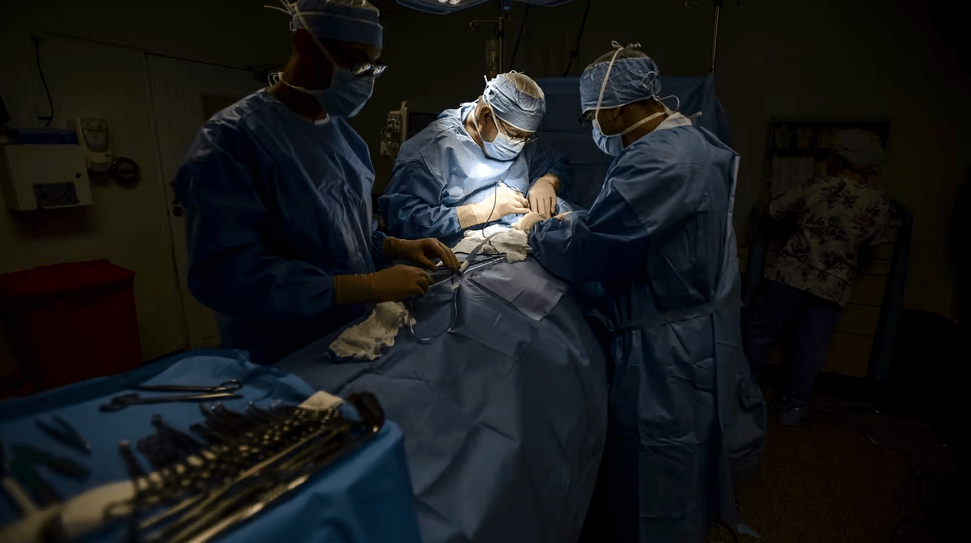
Photo credit: Carlos Giusti / AP
The aftermath of the hurricanes went beyond physical health to impact people mentally, with several women experiencing trauma, depression, and anxiety. Participants who already had children noticed concerning changes in their children’s behaviors and moods, and saw their kids become more attached to them. Some children ended up needing treatment to deal with their attachment issues.
When it came to accessing basic services, participants experienced no increased attention or care, despite their pregnancies, and stood in lines for food and gas for hours. At work, participants received no consideration for how their condition could affect their work. This finding demonstrates how disaster recovery often only focuses on the immediate needs of the general population, and does not take into consideration the kinds of healthcare needs for vulnerable groups of people. The services pregnant and postpartum women and their newborns need goes overlooked. Recovery plans should implement interventions that address specific health needs, which will make emergency preparedness better at responding to diverse communities.

Photo credit: Hector Retamal / AFP / Getty
The analysis also found that protective factors, such as interpersonal relationships and aid from organizations, were important in the recovery process. Participants benefited when they received materials and aid from their municipality, their jobs, or PROTECT. As support from the government was lacking, participants also noted a greater sense of community with those around them. These protective factors are important to consider in emergency preparation. Individuals, communities, and the government have distinct roles regarding support and access to resources. Emergency response research and implementation can take this into consideration to create more well-rounded, effective plans.
Participants deal with pregnancy and resource challenges on top of dealing with superfund contamination, which studies show is exacerbated during and after hurricanes. It is vital that better emergency response procedures are put in place to diminish some of the major burdens Puerto Ricans face following hurricanes.
