Project 2
Toxicant-Stimulated Disruption of Gestational Tissues with Implications for Adverse Pregnancy Outcomes
Pregnant women are exposed to a large number of environmental contaminants. These chemicals have the potential to compromise health of the mother and fetus by disrupting functions of critical tissues that support pregnancy. The placenta is one of these critical organs of pregnancy because it allows the exchange of nutrients, waste products, and oxygen between the mother and fetus. The placenta is also an essential source of hormones necessary for a healthy pregnancy and delivery. Because blood is delivered to the placenta at a very high rate, toxicants are efficiently delivered to the placenta once they are absorbed from the environment into the blood of a pregnant woman. Extending from the placenta, extraplacental or fetal membranes (“membranes”) form the gestational compartment that encloses the fetus and amniotic fluid. These membranes provide structural support and help protect the fetus from infection by bacteria and other microorganisms. Not surprisingly, premature rupture of these membranes leads to preterm birth. Exposure to bacteria and some toxicants can trigger release of signaling molecules from the placenta and membranes that stimulate onset of labor. The placenta and the membranes may be particularly sensitive to bacteria and pollutant disruption in the third trimester of pregnancy as the uterus prepares for labor.
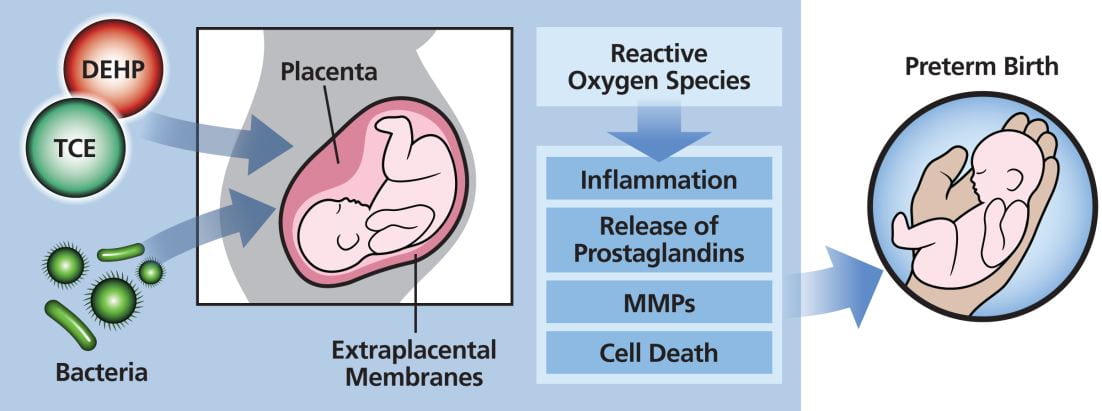
In Puerto Rico, where contamination with Superfund chemicals is extensive, the preterm birth rate is 11.4%, well above the U.S. average of 9.9%. Puerto Rican pregnant women have elevated exposure to several phthalates – chemicals used in plastics and personal care products – that are associated with preterm birth. In addition, exposure to the industrial chemical trichloroethylene (TCE) is a health concern for pregnant women because of significant groundwater contamination and its link to decreased birth weight. This project studies Superfund chemicals relevant to Puerto Rico, including the phthalates di-(2-ethylhexyl) phthalate (DEHP) and the structurally related di-(2-ethylhexyl) terephthalate (DEHTP), and trichloroethylene (TCE). Notably, there is scarce knowledge about DEHTP impacts on pregnancy, despite its increased use as an alternative to DEHP. Similarly, little is known about the ability of toxicants to modify bacterial infection of the placenta and the membranes, and subsequent health consequences.
This project contributes to the mission of PROTECT with toxicological studies of disruption of the placenta and the membranes as potential mechanisms of preterm birth and decreased birth weight. Experiments use tissue cultures of human placenta and membranes from healthy Cesarean deliveries as experimental models that allow manipulation for toxicity assessment. Specifically, we are using these experimental tissue culture models to understand how oxidative stress plays a role in placental tissue function disruption and susceptibility of membranes to infection with the bacterium Group B Streptococcus (GBS). The proposed studies will expand knowledge of phthalate and TCE toxicity to placenta and the membranes, providing new insights into stimulation of oxidative stress and inhibition of gestational tissue resistance to bacterial infection as biological mechanisms by which environmental contaminant exposures increase risk for preterm birth. By working with primary human tissue culture models relevant to late preterm birth – which accounts for most of the increase in preterm births in the United States – these findings have the potential for translation to medical and public health interventions with a significant impact on reducing preterm births.

Sean Harris
University of Michigan
Project Leader
harrsemi@umich.edu

Kelly Bakulski
University of Michigan
Project Co-Leader
bakulski@umich.edu

Chuanwu Xi
University of Michigan
Environmental Health
cxi@umich.edu

Rita Loch-Caruso
University of Michigan
Toxicology
rlc@umich.edu
